Colorectal Cancer
WHAT IS COLORECTAL CANCER?
Colorectal Cancer is a malignant growth arising from the colon or rectum. Benign (noncancerous) growths known as polyps may appear within the colon and rectum with age. Over time, these growths (polyps) can turn malignant and develop into cancer.
Most patients diagnosed with colorectal cancer are older than 50 years old. Patients who were diagnosed at an early age (before 40) may have a hereditary form of colorectal cancer.
WHO IS AT RISK?
Age: The incidence of colorectal cancer increases in those of age 50 and above.
Personal History: Patients who have been diagnosed with colorectal polyps or cancer.
Family History: Chances of developing colorectal cancer are higher in patients whose relatives have been diagnosed with colorectal cancer or genetic colorectal cancer syndromes. Eg. Familial adenomatous polyposis (FAP) or hereditary non-polyposis colorectal cancer (HNPCC).
Diet: Patients on a diet low in fibre and/or high in fat are believed to be at higher risk of developing colorectal cancer. Consumption of alcohol and tobacco smoking are also linked to increased risk of developing colorectal cancer.
Inflammatory Bowel Disease: This refers to a group of conditions including ulcerative colitis and Crohn’s disease. These conditions result in chronic inflammation in the colon and/ or rectum.
WHAT ARE THE SYMPTOMS?
- Blood in the stools
- Abdominal pain or discomfort
- Anemia (low blood count)
- A change in your usual bowel habit (pattern)
- Unexplained loss of appetite and/or weight
SCREENING TESTS FOR COLORECTAL CANCER
Faecal Occult Blood Test (FOBT) is a test used to check stool samples for occult blood. Occult blood in the stool may indicate the presence of cancer or polyps in the colon or rectum.
Double Contrast Barium Enema is a procedure in which x-rays of the colon and rectum are taken after a liquid containing barium is introduced into the rectum. This outlines the colon and rectum on an x-ray and helps to demonstrate abnormalities.
TYPES OF DIAGNOSTIC & STAGING TESTS FOR COLORECTAL CANCER
Colonoscopy is an investigation that allows doctors to evaluate the inner lining of your large intestine (rectum and colon). The colonoscope is introduced via the anus to look for ulcers, colon polyps, tumors, and areas of inflammation or bleeding.
* This is the gold standard diagnostic test for colorectal cancer
Computed Tomographic scan makes use of computer-processed combinations of many X-ray images taken from different angles to produce cross-sectional images of specific areas of a scanned object. In this case, it involves the torso.
* This serves as a staging investigation for colorectal cancer
Magnetic Resonance Imaging (MRI) is a type of scan that uses magnetism and radio waves to build up a picture of the inside of the body. An MRI scan shows how deeply the tumour has grown into body tissues. It can also be useful for assessing treatment response.
* This serves as a staging investigation for rectal cancer
Positron Emission Tomography (PET) – Computed Tomography (CT) scan is an important cancer imaging tool, as it serves both diagnosis and staging purposes, and provides prognostic information based on response.
A PET scan creates pictures of organs and tissues in the body by making use of the small amount of radioactive substance that will be injected into your body. Organs that use more energy; such as cancer cells, pick up more of this radioactive substance.The CT section of the scan shows where the substance is in your body.
A CT scan uses X-rays to create a three-dimensional picture of the inside of the body. It shows anything abnormal, including tumors.
* This serves as a staging investigation for colorectal cancer
Carcinoembryonic antigen (CEA) assay test measures the level of CEA in the blood. CEA is released into the bloodstream from both cancer cells and normal cells. When found in higher than normal amounts, it can be a sign of colon cancer or other conditions.
* This serves as a staging investigation for colorectal cancer and not as a screening test. CEA test should only be used after the diagnosis of colorectal cancer has been made. Approximately one third of colorectal cancer patients have normal CEA levels.
STAGES OF COLORECTAL CANCER
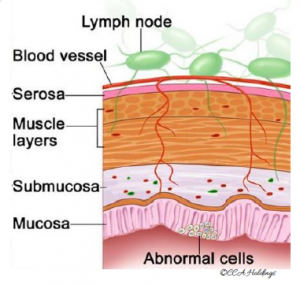
Stage 0 (colon carcinoma in situ)
Abnormal cells are shown in the mucosa of the colon wall.
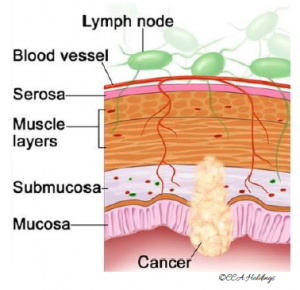
Stage 1
In stage 1, cancer has formed in the mucosa (innermost layer) of the colon wall and has spread to the submucosa (layer of tissue under the mucosa) and even up to the muscle layer of the colon wall.
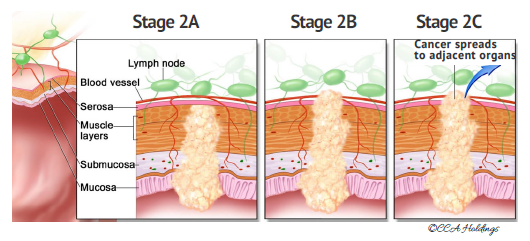
Stage 2
In stage 2, cancer has spread through the muscle layer of the colon wall to the serosa (outer most layer of colon wall).
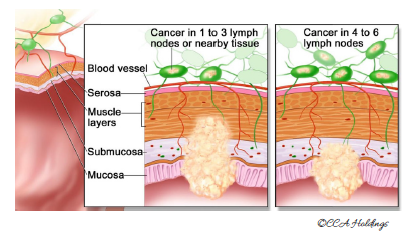
Stage 3
Cancer has spread through the mucosa of the colon wall to deeper layers. More importantly, the regional lymph nodes of the colon will have been involved with cancer in this stage
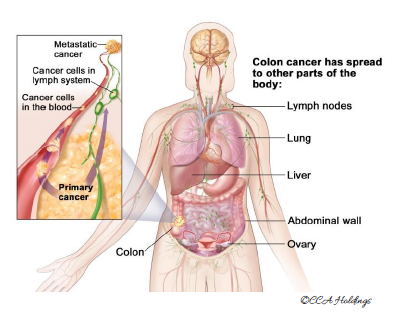
Stage 4
The cancer has spread through the blood and lymphatics to distant parts of the body, such as the lung, liver, abdominal wall, or ovary.
HOW ARE CANCERS OF THE COLON AND RECTUM TREATED?
Colorectal cancers are removed surgically through an abdominal incision. The affected section of the bowel is removed along with the associated blood vessels and lymph nodes. Upon removal of the affected section, the bowel is then reconnected (Anastomosis) to restore normal bowel functions. If the cancer has spread, chemotherapy and/or radiation therapy may be required.
Our surgeons predominantly employ a minimally invasive approach to perform these operations. The conventional open method of surgery practice is only performed in selected patients.
Types of Surgical Approaches
Laparotomy is a procedure involving a large incision through the abdominal wall to gain access into the abdominal cavity.
Laparoscopic Surgery, also known as minimally invasive surgery (MIS) or keyhole surgery, is a modern surgical technique in which operations are performed through small incisions (0.5–1.5 cm)
The advantages of laparoscopic surgery include:
- Reduced pain
- Shorter recovery time
- Shorter hospitalization
- Less wound and pulmonary complications
Robotic Surgery allows surgeons to perform complex procedures with more precision, flexibility and control than is possible with conventional techniques. It is a minimally invasive procedure performed through tiny incisions.
Chemotherapy may be recommended for advanced colorectal cancers, in which the cancer cells have spread to the lymph nodes or to other organs.
Radiation Therapy is employed mainly in the treatment of rectal cancers, either before or after surgery. The goals are to reduce recurrences or shrink the bulk of the tumour.
HOW CAN YOU PREVENT COLORECTAL CANCER?
Regular screening is key in detecting colorectal polyps or cancer early. The recommended age for commencing screening is 50 years old in individuals with no symptoms. Colonoscopy with the removal of polyps serves as the gold standard for the prevention of colorectal cancers.